
ICU WITH TARPS AND PLASTIC BAGS, TRIP 2, DAY 8
I’ve been in the ICU for a few shifts now. I’ve transitioned back into night shift, but I got a few shifts with the day staff, so I got to experience ICU rounds. Rounds are unique right now; the only person going into the room is the attending doctor overseeing the entire department. They’re putting their cell phones into a plastic zipper bag, turning it on speakerphone, and having one of us call them and place them on speakerphone as well. They’re discussing their physical exam findings with our discussion on the patient’s data, and we’re formulating a plan over speakerphone. It’s designed to reduce staff exposure to COVID, as every patient in this ICU has it, but it’s very stressful because we’re shouting information back and forth via a cell phone. I’m pretty glad to be back on night shift.
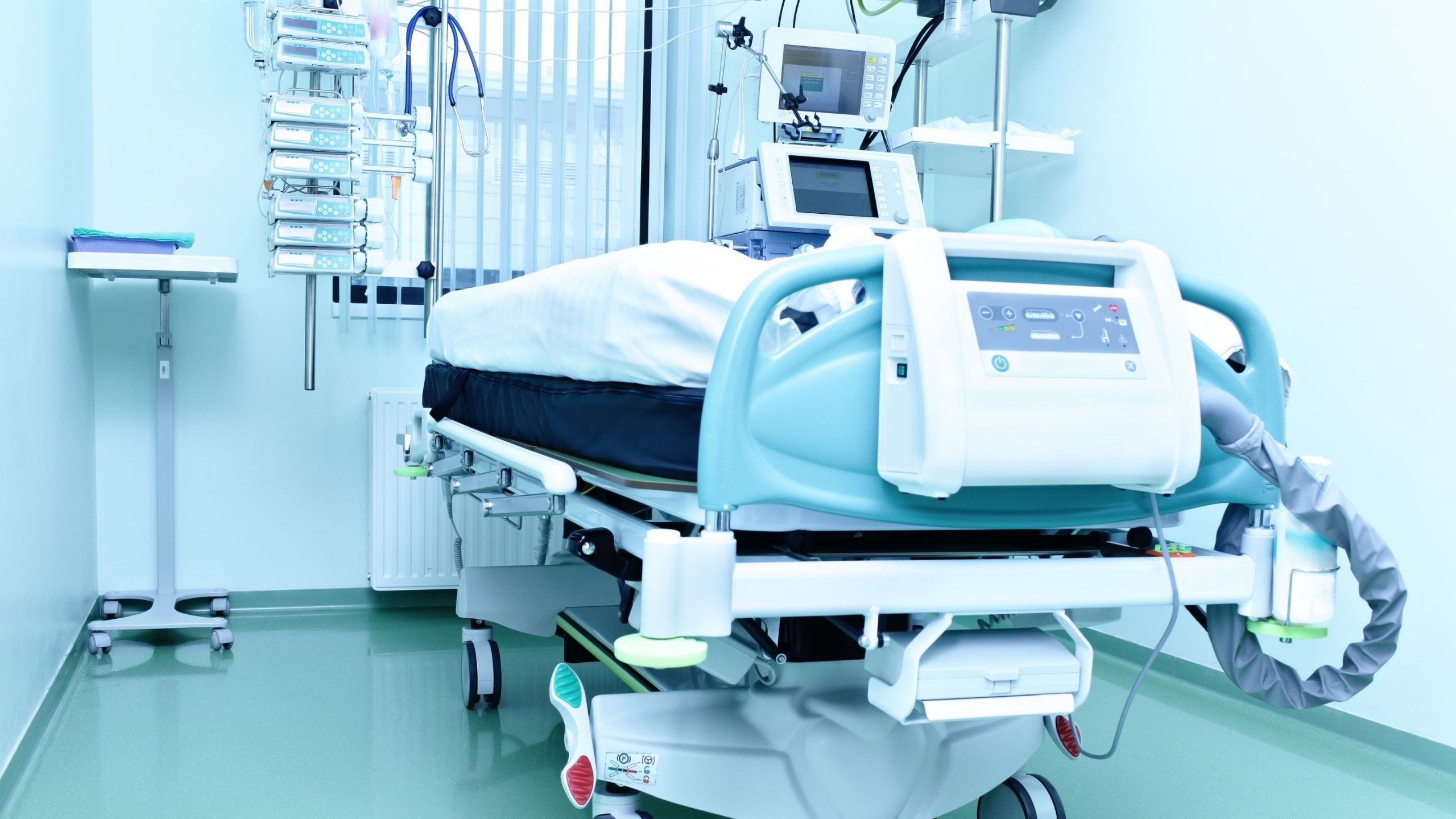
We spend most of the night shift making sure tasks get done and putting out fires. We’ve gotten a few transfer patients who needed blood transfusions or to be intubated on very short notice, but all in all night shift is a lot calmer than days. I’m an absolute fish out of water in this department. While I do know how to do most of the things here, I am only accomplishing perhaps ¼ or ⅓ of what one of their regular providers would. The charting system is one I’ve never used before and it’s taken me several days to really get used to it. Critical care medicine is not the same in an ICU as it is in an ED, though there are enough similarities that I can squeak by. I have a lot less autonomy here than I do in the ED, where I was basically running my own show. I’m frankly a lot more comfortable with less autonomy in this setting; I can manage emergencies well, but long-term planning is just not my wheelhouse and it’s going to take some time before I adjust to the thought process.
During day shift rounds, I’m expected to understand and be able to verbalize the entirety of the plan of care to date; the rationale behind that plan of care; all of the labs, previous medications, and other interventions; and then help synthesize plan changes. We don’t do a formal set of rounds on nights or make major changes to the plan, thankfully, but I still need to know those things to make good decisions when someone needs an abrupt change of plans (usually due to deterioration). Often those good decisions are absolutely contrasted with the previous plan of care, and that’s okay on a short-term basis. Many patients are being tapered off their paralytics on the day shift, for example, and are put right back on them on nights to keep the patients from straining their systems and wasting their bodies’ resources by fighting against and choking on the ventilator, particularly at night. It’s uncoordinated and ugly, but we’re getting things done anyway. Part of the disconnect is just the day/night perspective change. We endeavor to maintain a normal sleep/wake cycle, so during night shift, we try to keep the patients asleep as much as possible. Due to constant interruptions in the ICU and the fact that many patients spend their daylight hours weaning off sedatives, we often have to change previous care orders to promote nocturnal sleep. Additionally, many people sleep in the prone position (on their stomach), which they often can’t do without at least a low dose of a paralyzing medication.
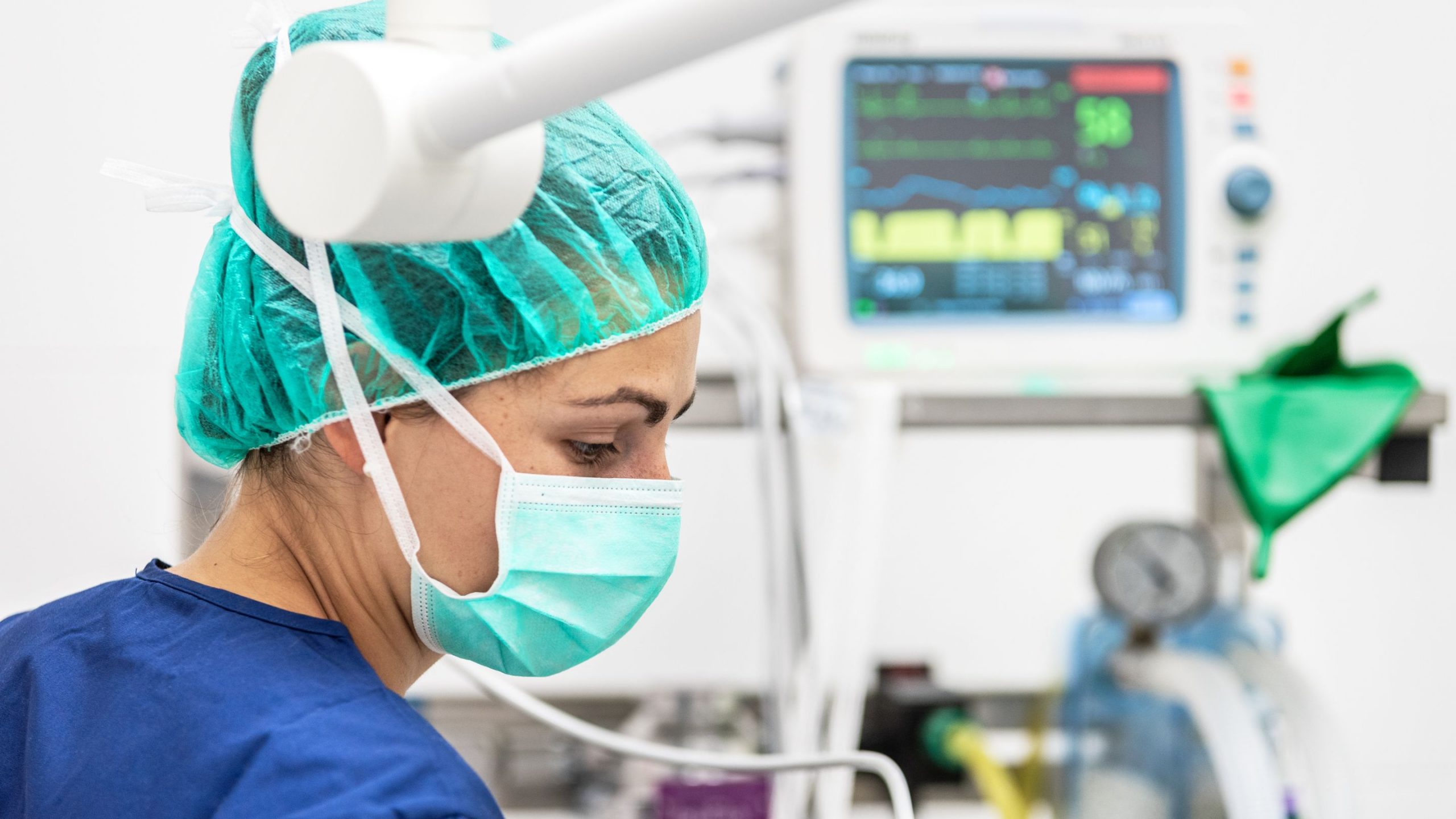
Much of the actual work I’ve been doing has been procedural or directly overseeing the nurses. I’ve been taking out expired vascular access lines, starting new IVs (this is the singular thing that I’m still the best in the department at), helping with intubations and extubations, and making sure tasks get done in a timely manner. I’ve been doing family conferences with families of patients I may or may not actually have any hand in the care of. In many cases, the patient is deteriorating and unlikely to live, and I get to explain that in understandable terms to family members of a patient who I’ve only seen through a plexiglass window in a construction tarp and done a brief chart review on. Some of the families are able to do video conferences with patients via an iPad on wheels, so I’ve been setting up and coordinating some of those visits.
I’ve pushed paperwork, getting consent forms and power of attorney forms signed. It’s all work that needs to be done and I’m certainly not above doing it, but I feel like a student again because my proficiency in doing everything is just not there. I still require a lot of direction to make sure everything is getting done correctly. I’ve been so used to being completely on top of what I’m doing that it’s actually very jarring to be a novice again. I feel like people are being patronizing when they say that I’m being helpful because my actual accomplishments in a 12-hour shift are less than half of what they’re able to do. I know nobody actually means it that way or thinks that, but I’m definitely projecting that less-than-useful feeling, as I’m far from competent or proficient in this setting.
JACKIE CHRISTIANSON
Author
Share this post
Nurses International is a non-profit entirely focused on helping nurses obtain the education and the support they need to make a difference in developing nations worldwide.
We connect colleges and institutions with experts who can take their nursing programs to the next level. We help establish new nursing programs where they’re needed most. And we eliminate the barriers that stand between students and education.
QUICK LINKS
CONTACT US
FOLLOW US
EIN: 46-4502500