
TRIP 3, JOURNAL #2
The last several days in the MICU have been fairly slow. They cleared the South side of the ICU for terminal cleaning starting on Tuesday, so our census has been very low to accommodate. They’re converting the MICU into a non-COVID area. It’ll be interesting to see how long that lasts. It’s only a matter of time until a COVID patient slips through the cracks and they have to close everything down and re-clean. After they closed for cleaning, I was moved to the newly exclusive COVID ICU. Most of the patients I had previously were moved here, but there are a few new faces, too. This area is normally an ICU stepdown but was upgraded to ICU-capable when we desperately needed the critical care beds. The patients up here are somewhat less sick than the MICU ones were but still precarious enough they need to be near ICU care if they deteriorate. They’ve all got similar lung injuries to what we saw in MICU, but to a somewhat lesser degree. There’s lots of scarring and fibrosis of the lungs and oxygen dependence, and most have been here for at least two to four weeks. I almost pity them more here. Most of these patients are alert and at least semi-aware of their surroundings, whereas the MICU patients were mostly sedated and (hopefully) amnesic.
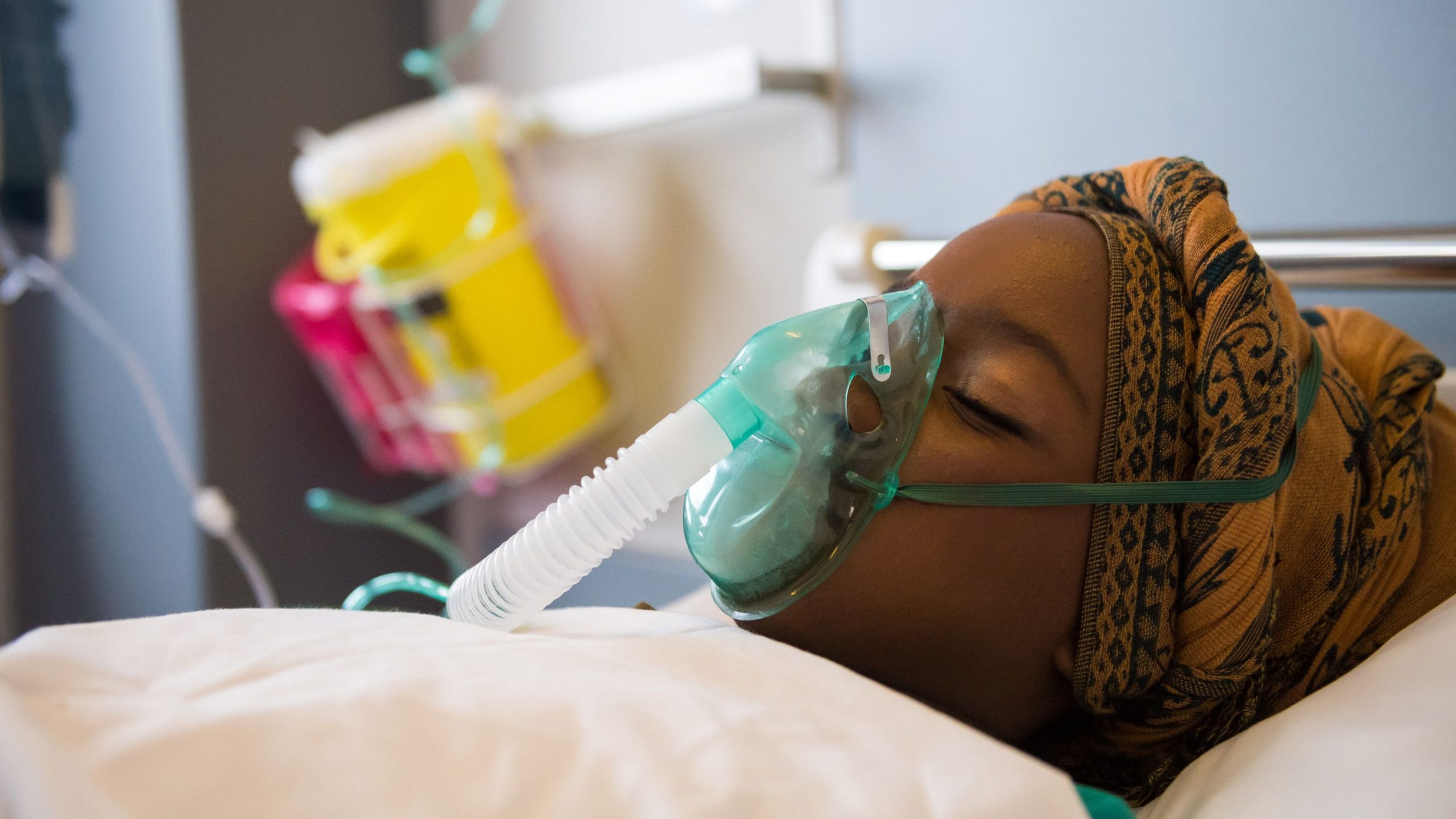
We had a new “success story” over the past week. A man in his early 50s who’s been in and out of our ICU was finally starting to improve. He’s been hospitalized for COVID for about two months straight. He’s been in ICU thrice throughout his hospital course; I’ve had him for both of his return trips. He came back to us because he had to be intubated for a third time. He went for a tracheostomy four days ago and he improved dramatically when we were able to reduce his sedation post-trach. He’s awake now, is completely cognitively intact, is off blood pressure support medications, and looks likely to make enough of a recovery to discharge to a long-term care setting. My guess is that he’ll be on a ventilator for the rest of his life, but he’ll probably live.
I learned this weekend that one of my colleagues is a fellow acrobat (and a considerably more skilled one than I am, at that). He’s more of a partner acrobat, which I’ve not done much of (as my own solo skills are pretty sketchy), but we decided to try a simple, short trick. He had my shoulders on his feet and I basically did a headstand with my shoulders balanced on his feet. We were going to try to convert that pose into a handstand, but the ceilings were barely high enough for the headstand version, so we couldn’t. The nurses allowed us to open the tent flap of the patient described above and do a brief performance for him. Then we did an encore round for the only other patient who was awake on the unit — a nice old man with Down syndrome who had also recently been extubated. (He was awake and seemed to enjoy it.)
Thus, the COVID Circus was born. We were able to practice but didn’t have a chance to perform for any patients the following night (they blessedly slept through most of the night), so we made a pact to do a new trick every shift we work together and hopefully do a brief show for the awake patients nightly. It’s totally frivolous and silly, but these people have been through hell and it takes perhaps 15 minutes to brighten their day. The nurses love it, too, and to be fair they’ve likewise been through hell. We even got a couple of the other PAs to try it. One was brave enough to try the partner headstand with spotters. A couple of other PAs who have never tried a handstand gave it a try with spotting and instruction, too. The videos of our stunts have spread around the hospital. Nurses on other units have been asking to see more tricks or other videos from my circus escapades prior to COVID. It’s nice to have a little joy on shift for a change of pace.

An idea that keeps me sane, in the wake of knowing many of my surviving patients will have comparably low qualities of life after COVID, is the concept of the hedonic treadmill. The broad idea is that life events may change one’s happiness short-term, but most individuals adapt to new situations and return fairly quickly to their previous baseline level of happiness. One of the more famous studies on this was one in the 1970s that followed about 60 people. One-third of them were new lottery winners, another third were people who had not experienced a major life event (a control group), and one-third were new spinal cord injury victims. In short, the study found that the lottery winners were happier and the spinal cord victims were much less happy in the short term, but the change in both groups was temporary despite the permanency of their respective life-altering events. There’s been subsequent research with similar findings, and there’s more nuance to the concept of the hedonic treadmill thanks to subsequent research today, but I’d like to think that research is relevant to the quality of life questions I have for some of these patients with new chronic illness. It’s objectively awful to spend the rest of your life on a ventilator, but perhaps they will adjust and still have fulfilling lives, much like the new paraplegics adapted.
JACKIE CHRISTIANSON
Author
Share this post
Nurses International is a non-profit entirely focused on helping nurses obtain the education and the support they need to make a difference in developing nations worldwide.
We connect colleges and institutions with experts who can take their nursing programs to the next level. We help establish new nursing programs where they’re needed most. And we eliminate the barriers that stand between students and education.
QUICK LINKS
CONTACT US
FOLLOW US
EIN: 46-4502500