
COWBOY MEDICINE TRIP #2, DAY 5
The past few days have been a roller coaster. I returned to NYC on Monday for a second contract (today is Friday). I was finally able to get a flight after having two cancelled on Sunday. I was scheduled to start on Monday for night shift, as I was contracted for 10 straight 12-hour shifts in the same facility. Things changed a bit during my layover. One of the ED directors called me and told me their volumes had significantly improved, so I was being reassigned to one of their Manhattan hospitals to work with inpatients. They gave us a sort-of option for where we could be assigned: if we had critical care experience, we had the option of either going to the COVID ICU or working in the long-term post-COVID ventilator unit. I will be primarily in the COVID ICU, though I asked to work a 12-hour shift every day that I’m out here, so I may float between the two to accommodate that schedule.
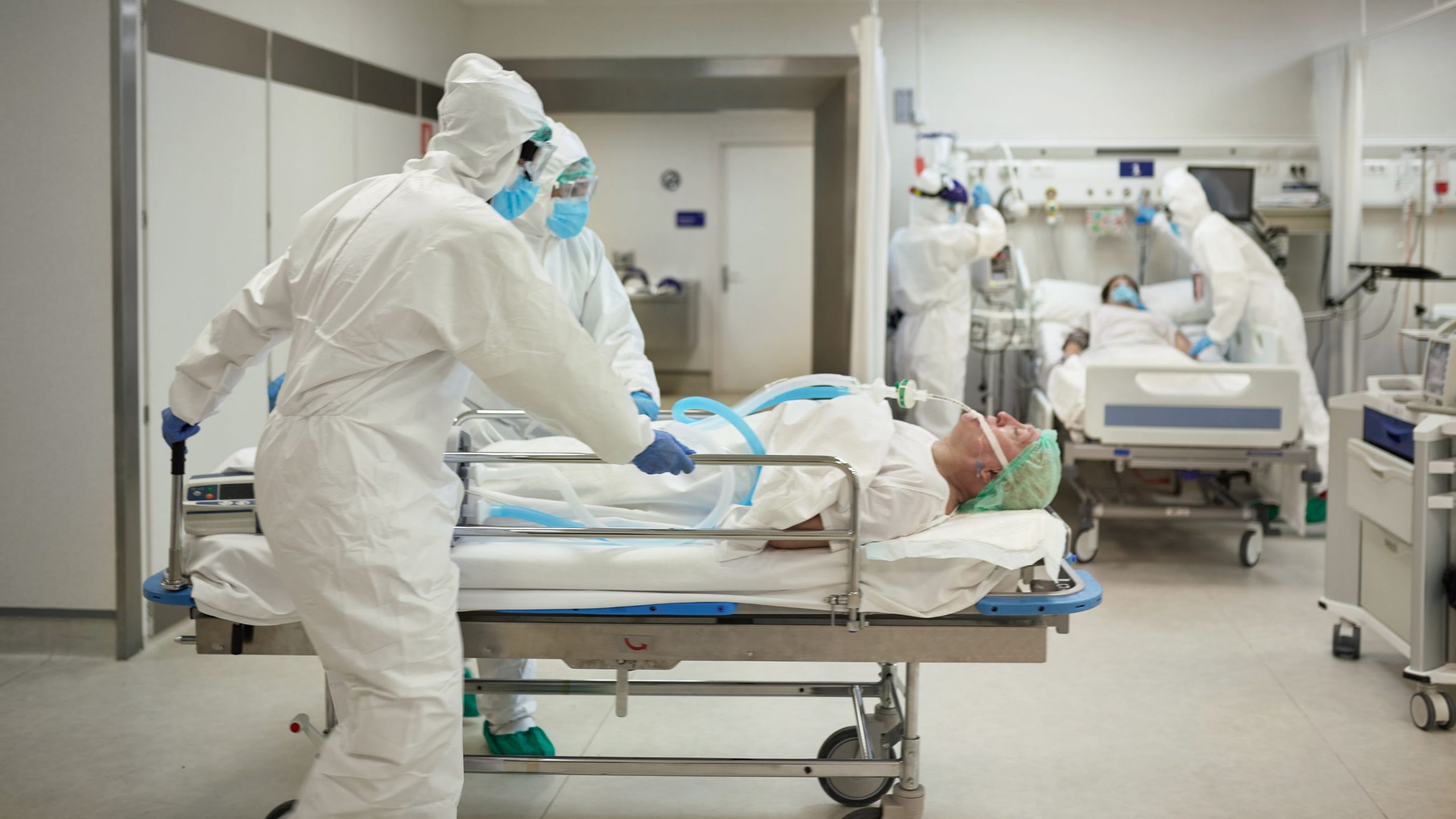
The situation at the hospital is evolving but fundamentally boils down to the following: The hospital had been trying to gradually cease operations in anticipation of a move to a new hospital building. Their previous capacity was about 850 beds but was down to about 200-250 staffed beds prior to COVID-19. COVID surge happened three weeks ago, and the hospital had to abruptly reopen those 600 beds. They had successfully opened three new ICUs for unstable patients on ventilators. They are now in the process of opening up a few long-term ventilator units. The long-term ventilator units are for patients who are alive and at least somewhat functioning, neurologically speaking — they are stable enough to be taken out of ICU, but can’t get off the ventilator. Those patients need a place to go so they’re not unnecessarily taking up ICU rooms and blocking out patients who need the treatments that can only be done in an ICU.
The long-term ventilator units are supposed to be operational in the middle of next week, pending some additional staff onboarding. My understanding is the long-term ventilator unit will be working toward managing and rehabilitating patients who are vent-dependent for more than two to three weeks. The damage to the lungs of most of our COVID patients is extensive, far beyond what a normal respiratory failure causes, so many are having difficulty going off the vent. Some of those long-term ventilator patients will end up on a ventilator for the rest of their life due to the damage to their respiratory system, and some may consequently never return to their homes. Some may be able to return home, perhaps vent-dependent only at night, but will need rehabilitation to relearn how to brush their teeth, walk, or perhaps even care for their own tracheostomies and ventilators. Others will have to undergo further surgeries to repair the tracheostomy and restore their previous airways.
These people have nowhere to go without a long-term vent unit, and they’ll likely be in the hospital for months. The hospital I’m at is expecting to keep these patients at least through June, possibly into July and later. I imagine other hospital systems are contending with the same issue — what do you do when COVID surge is over, you’ve got thousands of people who are alert and cognitively intact, and you can’t take them off the ventilator? What happens if your ICUs and vent units are full and a second surge happens because the state has released shelter-at-home restrictions? I wonder what the death toll will be like during the second surge, when we’ve absolutely exhausted ICU resources.
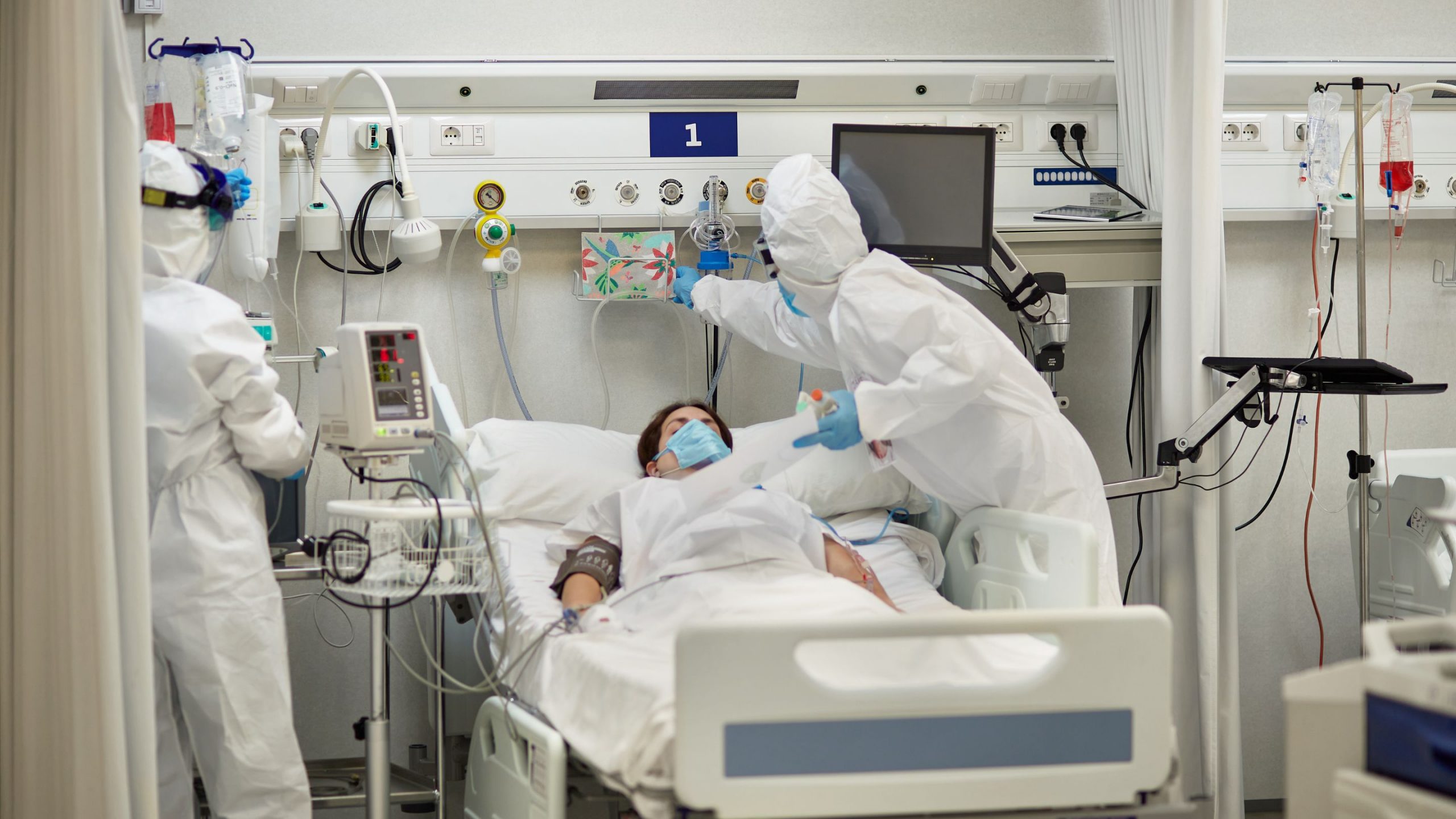
The COVID ICUs are a world unto themselves. The staff safety is significantly better in the ICUs; COVID patients are recommended to be in negative-pressure rooms (rooms in which the air pressure is less than the rest of the building, to prevent the infected air from seeping into the rest of the building and infecting others). The ED can’t even come close to accommodating this necessity, but ICU has managed to. All of the rooms have been haphazardly converted into negative-pressure rooms, some using plastic-zippered construction tarps and fans. All of the ICU patients are undergoing experimental treatments. Some of the treatments are being studied and trialed, but none of them are proven or even established to be effective. The risk of possible death isn’t so high when the alternative is almost certain death, so they’re receiving those unstudied treatments despite the risk. Nothing is by the books because there isn’t a book on this, and the treatments recommended by the books we had before make the disease complications so much worse. It’s truly cowboy medicine.
JACKIE CHRISTIANSON
Author
Share this post
Nurses International is a non-profit entirely focused on helping nurses obtain the education and the support they need to make a difference in developing nations worldwide.
We connect colleges and institutions with experts who can take their nursing programs to the next level. We help establish new nursing programs where they’re needed most. And we eliminate the barriers that stand between students and education.
QUICK LINKS
CONTACT US
FOLLOW US
EIN: 46-4502500